Postpartum depression or postpartum thyroiditis?
My own experience with postpartum depression started 6 weeks after the birth of my first child, Annika. I remember clearly that it was a Friday, Annika was “colicky” (or so they said) and had one of her fits of crying that lasted about 45 minutes. Me, I cried for three hours straight.
Before having Annika I knew I was passionate about treating children with naturopathic medicine, but it wasn’t until I became a mother that I realized the need for treating moms as well.
Treatment of postpartum women is a huge part of my practice here in Missoula. It is sadly underreported, undertreated and frankly I have found conventional medicine to have very few treatment options available for women who don’t want pharmaceuticals.
That’s why I have devoted a percentage of my practice time to research and making videos and blog posts to help women with PPD. (10-15% of postpartum women!)
My approach to PPD treatment (just like my approach to treatment of many other conditions) is to figure out the underlying cause. I’ve got to tell you, in my practice probably 9/10 times my patients that come in to me with depression have something else going on. In fact, I’ve never seen normal lab values in a patient with depression. That’s because depression happens quite frequently ANY time the body runs out of resources. You have iron-deficiency anemia? Guess what, you’re oxygen deprived and you will feel awful. You have kidney problems? Guess what, your body can’t keep a correct electrolyte balance! You have intestinal problems/dysbiosis? Guess what, you can’t absorb nutrients like B vitamins to keep your cells running. (I will talk about these other problems in more detail in future episodes.)
Ditto for thyroid gland problems.

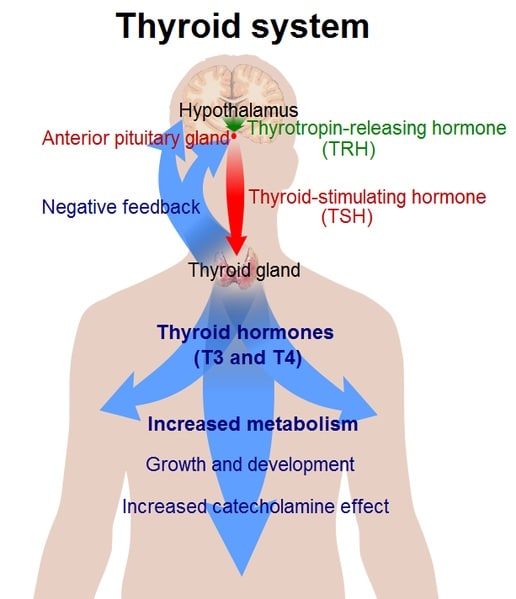
So here is the thyroid gland. It is a little hormone-secreting gland that sits in the front of the neck, you can gently touch the gland right underneath your adams apple. It normally enlarges in pregnancy because you need extra thyroid gland to support you and your baby.
The thyroid gland basically sets the metabolic rate for the entire body. That’s why people who have too much thyroid (called HYPER thyroid) feel like they’ve had too many cups of coffee. If you have LOW thyroid you typically feel sluggish, fatigued, depressed, and often have dry skin, hair, nails. Basically if you don’t have enough thyroid gland your cells don’t have enough energy to operate. It is no surprise that someone with low thyroid gland function would feel fatigued!!!
More about the thyroid gland: 1) it requires iodine to make thyroid hormone. This is why women should keep taking moderate levels of iodine (like a good quality prenatal) even in the postpartum period. Do NOT take excess iodine. 2) it is inhibited by soy, peanuts and uncooked Brassica vegetables (like broccoli, cauliflower, kale, etc). This is a bit overblown in popular media – it is only raw veggies that really significantly affect thyroid function (in very large amounts). 3) it requires a protein to shuttle the hormone around to various places in the body.
Measuring thyroid gland. Most physicians will screen you for thyroid problems by using TSH (thyroid stimulating hormone). It is confusing for people because a HIGH TSH means you have LOW thyroid gland function. TSH is what the pituitary gland secretes. (it’s in the brain. Yes, it looks suspiciously like a member of the male anatomy, only much much tinier). It is the brain saying “hey, there’s not enough thyroid hormone, we need more”. The thyroid gland itself receives that message and is supposed to make more. BUT if it CAN”T produce more then the TSH will keep going up and up.
You need to test more than just TSH. Some doctors will only test TSH – this is a mistake. Normal low thyroid (hypothyroid) conditions have a high TSH and low T3/T4 (thyroid hormone) – but not everyone has a “normal” thyroid condition! As a natuorpathic physician I want to know the levels of your thyroid hormone (T3/T4), plus the amount of binding protein (thyroid uptake or TU), the amount of free hormone (FTI or free thyroxine index), and maybe even a measurement of how thyroid gets converted (reverse T3 or rt3 – a measurement of degradation of the hormone).
Then we need to know if there is an autoimmune condition happening. Postpartum thyroiditis affects 5.4% of the general population! Whoa!
Postpartum thyroiditis has a variable course. Some women fluctuate between hyperthyroidism and hypothyroidism. (This is why it is so challenging to treat!)
The symptoms of hypothyroidism include fatigue, depression, cold intolerance, thinning hair/nails, dry skin, and a feeling of “slowness.” In hyperthyroidism many women feel anxiety, fatigue (like a “burnout” fatigue) restlessness, palpitations, migraines and more.
Autoimmune thyroid conditions are diagnosed by measuring antibody levels. Anti-TPO and Anti-TG are antibodies against different parts of the thyroid gland (or, rather, different parts of the process of making thyroid hormone). Anti-TPO is usually king, but if I am really suspicious I”ll order an anti-TG too.
Treatment for thyroiditis. “Selenium decreased the incidence of PPT as well as permanent hypothyroidism when compared with a placebo control group.” I like selenomethionine the best for treatment of autoimmune thyroid problems. Antioxidants are huge – turmeric, by the way, has been shown to help many inflammatory conditions, including pain! I recommend liberal amounts of turmeric to be eaten with food to decrease inflammation and possibly help with autoimmune conditions. It needs to be eaten with fats for best absorption. Probiotics are one of my favorite immune modulators – but you MUST MUST MUST get a high quality probiotic, not the junk that is sold over the counter at a supermarket. (Culturelle brand is pretty good, you can find it most places. I have a few others that I really like that I carry in my office. Honestly, the rest is garbage.)
I do a lot of treating intestinal dybiosis too – it contributes to the general antigenic load which can stimulate autoimmune conditions.
Oh, and yes, the emotional component. I have yet to see an autoimmune patient without some sort of emotional component. That is one of the greatest parts about being a naturopathic physician – we recognize that healing occurs on so many levels all at the same time.
I hope this was helpful! Please comment below if you have experienced postpartum depression that was due to postpartum thyroiditis or hypothyroidism. I would love to hear your stories.








Maggie Luther
August 13, 2013 at 11:01 amThanks Dr K
What a wonderful explanation of the overlap in similarities of pp depression and thyroid disease. Love the slideshow. I agree that most probiotics are best bought at a coop or whole foods type store to make sure you get a good source. Lactobacillus is super important for the small intestine (like culturelle) whereas Bifidobacterium species are so important for the large intestine/colon. Getting a product with both genus and multiple species is the best bet for a quality product.
Thanks,
Maggie
Claudia Guy
August 25, 2013 at 7:16 amThanks Dr. Krumbeck,
This is well explained and in simple terms. I’m glad to see this very common condition addressed. PPT or PPD is so much more common than we admit. Addressing this, in effect, helps families. If fact, preventing PPT is probably best.
Is there hope that PPT is reversible, or does the practitioner continue to manage it as an autoimmune disease?
Dr. Erika Krumbeck
August 25, 2013 at 11:29 amFor a subset of women with PPT the thyroiditis continues as a lifelong hypothyroid condition – which allopathic medicine treats with thyroid hormone medication continuously. I am hopeful that if naturopathic medicine can address the underlying cause early enough that we can prevent much of the permanent damage that occurs, and thus reduce the need for lifelong hormone. I think it is also critical to try to identify women before conception and treat inflammation and autoimmune disease early. Remember to treat the individual, not the disease!
Catherine R
December 14, 2014 at 7:26 amI thank God that I have found this. I thought I was losing my mind. I am now 6 months postpartum. I had a 2 litre blood loss when delivering my daughter and developed iron deficiency anaemia afterward. Took Iron tabs for 8 weeks but still felt very fatigued. Full blood count showed my iron levels had recovered and to cease iron therapy. The fatigue continued (almost to the point of being unable to function!) and was accompanied by vertigo and dizziness. I began to panic due to this and had anxiety headaches, lack of appetite and shortness of breath. Admitted to hospital did a full blood count and lung scan and nothing wrong. I mentioned thyroid testing to a doctor – it was dismissed and I was diagnosed with Postpartum Anxiety/Depression and given a prescription for antidepressants. I’ve now been on SSRI antidepressants for four months and feel like I’m on an emotional rollercoaster … One week I am fine mood-wise then feel down, then fine the next, followed by an anxious week. I feel the moods are hormone related – ovulation and week prior to AF – as I have no control over them. I also suffer from eczema, itchiness, carpal tunnel, night sweats, cold sweats, plantar fasciitis, irregular periods, mid-cycle bleeding and tingling in throat and tongue.
Is it worth going back to my GP and demanding a thyroid test? The only solution my doctors seem to have is increasing my Celexa/Citalopram. I have already doubled my dose and it made no difference.
Another thing that came up with my symptoms is Sheehan’s syndrome but it does not seem related to mood disturbances and vertigo (my main symptoms) and the fatigue I experienced initially has gone.
Reading your article here has been a lightbulb moment for me as I feel like the more i research PPT the more it seems to fit. I feel I’ve been at my wit’s end and no one has been listening to me. They just think I’m in denial of Postpartum depression/hormonal when my instinct is screaming at me that something is wrong with my body. I intend to go back to my doctor and tell them about PPT and that I need to have my thyroid hormones tested.
All best ( and thank you for this site)
Catherine (UK)
Dr. Erika Krumbeck
December 15, 2014 at 10:27 amHi Catherine,
I think it is always worth it to get a thyroid test and to investigate Sheehan’s syndrome. Make sure they check your iron levels, too – a ferritin is the best test.
– Dr. Erika
Kira
December 5, 2015 at 3:45 amI know this is from a year ago but I’d love to hear how you went Catherine! I stumbled upon this because PPT fits my symptoms too and I have had thyroid testing done, my levels have just gone hypo after 3 months of weight loss, loss of appetite, dizziness, shortness of breath, heart palpitations that all started with vertigo. I am also aware that my antibodies are higher than they should be, not extremely high but they are present which makes my risk for PPT higher. You are the firsr one I have come across with 100% the same symptoms as me with the dizziness and everything so I’d love an update!
trish
March 1, 2016 at 8:48 pmI think I have been dealing with this too. Were you hyper for 3 months? I started being hyper in Dec. And the symptoms have improved drastically but are still there. Its been almost 3 months. I didn’t know hyper could last this long.
Leslie
June 17, 2015 at 1:02 pmThank you for all of this information. I am 4 months post partum and have had a thyroid condition for 12 years. I take Synthroid. My doctor’s keep telling me my thyroid level is normal but I suspect post partum thyroiditis. I have insomnia, severe fatigue, anxiety, palpitations, I lost all of my baby weight within a week of giving birth and am now 10 llbs under my normal weight which all of my doctors have dismissed. Emotionally I feel depressed, overwhelmed which has really preventing me from bonding with my baby or enjoying him. I’m frustrated that I am not getting any answers. If I have ppd I want to deal with that but I would like to rule out post partum thyroiditis first or any underlying conditions or hormonal imbalances. I don’t want to take antidepressants if I don’t have to.
Cindy Sundvik
June 28, 2016 at 8:39 pmI too had the same situation 29 years ago. The doc’s said they checked my thyroid and said it was “normal”. Back in the day they knew so little about testing the thyroid. Anyway, I fought and fought to get out of my PPT by myself. Years later and another baby later, I was finally diagnosed. See a homeopathic or naturalistic doc who will do all the tests needed (D, iron, all thyroid tests, hormones, and more) and you will find the answer.
My heart and prayers are with you. It’s a struggle. There is an answer.
Shine on!
Kendra
August 9, 2016 at 5:44 pmCan you review my info. I am confodent I have this but my Dr is stringing me along.
Melissa Siegrist
September 21, 2017 at 7:04 amHi there! Thank you so much for explaining this so clearly. My TSH was 0.06 and as of last week it is 2.2. My baby is 10 months old now and it took that long to normalize. I am a weepy mess and still hot and tired. My period was also a week late when it’s normally 28 days on the button. I cannot find a endo doctor that I like Or one that calls me back. Any advice would be great, even if you tell me that I’ll feel better soon. Thank you!